Introduction
Juvenile Open Angle Glaucoma (JOAG) is a rare but serious condition that affects children and young adults. If left untreated, it can cause permanent vision loss. Understanding its symptoms, causes, and treatment options is essential for early detection and effective management. This guide explores the key aspects of JOAG, from warning signs to treatment and daily management strategies.
Symptoms of Juvenile Open Angle Glaucoma
A. Early Warning Signs
- Eye discomfort: A feeling of eye pressure or mild pain that can be mistaken for fatigue or strain.
- Halos around lights: Blurred or distorted vision accompanied by halos or rings around lights may indicate JOAG.
B. Progression of Symptoms
- Loss of peripheral vision: Gradual loss of side vision, often described as “tunnel vision.”
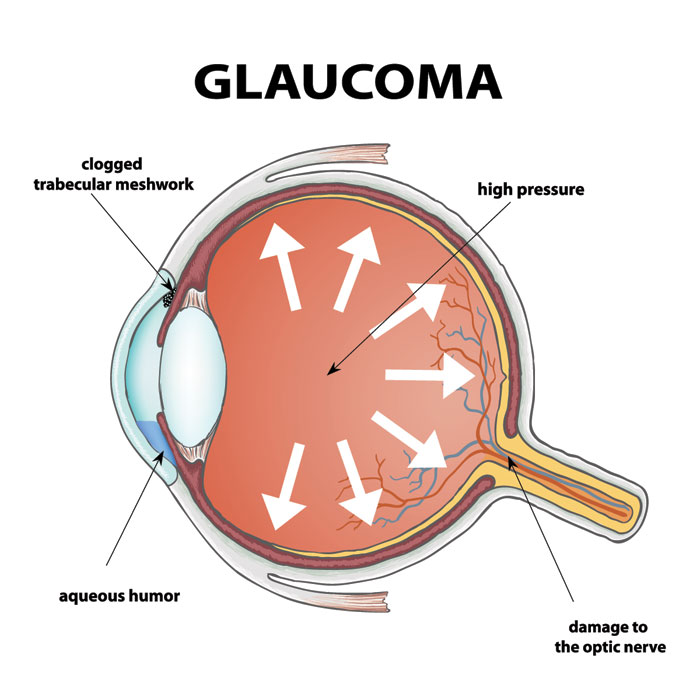
- Increase in intraocular pressure (IOP): Elevated eye pressure that can damage the optic nerve, leading to vision loss.
Causes of Juvenile Open Angle Glaucoma
A. Genetic Factors
- Family history: A strong family history of glaucoma significantly raises the risk of JOAG.
- Gene mutations: Mutations in genes like MYOC, OPTN, and TBK1 are linked to this condition.
B. Environmental and Health Factors
- Eye injuries: Previous injuries or infections may contribute to glaucoma development.
- Underlying conditions: Juvenile diabetes, high blood pressure, and other ocular issues can increase risk.
Diagnosing Juvenile Open Angle Glaucoma
A. Medical History and Eye Exams
- Regular check-ups: Routine eye exams, especially for at-risk individuals, are vital for early detection.
- IOP measurement: Consistent monitoring of intraocular pressure helps identify problems early.
B. Diagnostic Tests
- Visual field test: Assesses peripheral vision loss, a common symptom of JOAG.
- Optical coherence tomography (OCT): Measures retinal nerve fiber layer thickness to track disease progression.
Treatment Options for Juvenile Open Angle Glaucoma
A. Medication
- Eye drops: Prostaglandin analogs, beta-blockers, and alpha-adrenergic agonists help lower eye pressure.
- Oral drugs: Carbonic anhydrase inhibitors or beta-blockers may be used when eye drops are insufficient.
B. Surgical Options
- Laser surgery: Procedures like trabeculoplasty and iridotomy improve fluid drainage and lower pressure.
- Trabeculectomy: Creates a new drainage pathway to reduce intraocular pressure effectively.
Lifestyle and Daily Management
- Stay active and maintain a healthy weight: Regular exercise supports overall eye health.
- Monitor eye health: Follow treatment plans and schedule frequent eye exams.
Living with Juvenile Open Angle Glaucoma
A. Coping and Management
- Adherence to treatment: Consistency in medication and follow-up visits is crucial.
- Support for vision loss: Seek help from low-vision specialists and occupational therapists for daily adjustments.
B. Emotional and Social Support
- Family and friends: Emotional support from loved ones can reduce stress and improve quality of life.
- Counseling: Professional mental health support can help patients cope with the emotional challenges of JOAG.
Final Thoughts
Early diagnosis and proper treatment of juvenile open angle glaucoma can prevent permanent vision damage. Raising awareness and continuing research are essential steps toward improving the lives of those affected by this condition.