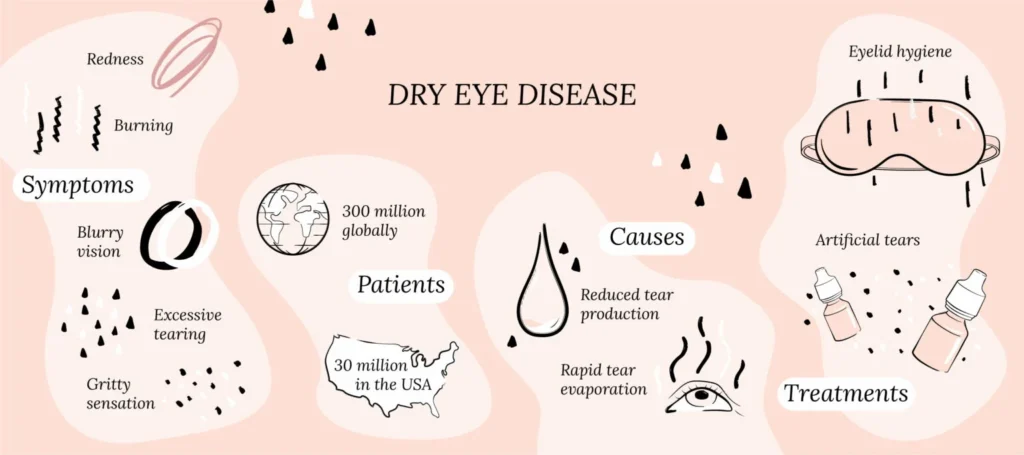
Simple Steps to Simplify Dry Eye Disease Diagnosis for Clinicians
Dry eye disease (DED) remains one of the most pervasive yet underdiagnosed conditions in optometric practice. The disconnect? Too many clinicians still rely on outdated or incomplete diagnostic frameworks. But here’s the reality: effective DED diagnosis doesn’t have to be a labyrinth. By adopting a streamlined, evidence-based approach, you can move from confusion to clarity—often in less than five minutes.
In this article, we break down actionable clinical steps to cut through the noise, identify the dry eye subtype, and initiate targeted therapy without overcomplicating the process.
Why Dry Eye Diagnosis Still Feels Complicated
Even with advanced diagnostic tools, many practitioners still feel stuck. Common issues include:
- Over-reliance on a single test (e.g., tear break-up time alone)
- Patient history that doesn’t match exam findings (symptoms without signs)
- Confusion between aqueous-deficient and evaporative dry eye
- Limited time for full diagnostic workups
The solution is a hierarchical, systematic approach that separates basic screening from advanced profiling.
Step 1: Master the Triage Questionnaire
Diagnosis starts before the slit lamp. A validated symptom questionnaire is your first step.
Common tools include SPEED and OSDI, but a faster version can include:
- Frequency: How often do you experience dryness, burning, or grittiness?
- Severity: Rate discomfort from 0–10 at the end of the day
- Triggers: Do symptoms worsen with reading, screens, or wind?
Key insight: Even “mild” symptom scores can indicate early-stage disease. Early intervention prevents progression.
Clinical Tip
If a patient says “I just have allergies,” ask about symptom type.
- Allergy: itching, watery discharge
- Dry eye: burning, foreign body sensation
Step 2: Perform the “Quick Three” Objective Tests
You don’t need extensive testing for every patient. Start with three high-yield checks:
Tear Break-Up Time (TBUT)
- Apply 2–3 µL fluorescein
- Ask patient to blink once, then hold eyes open
- Measure time until first dry spot appears
Interpretation:
- <10 seconds = abnormal
- <5 seconds = severe instability
Low TBUT with normal tear volume suggests evaporative dry eye (often MGD).
Corneal and Conjunctival Staining
- Use fluorescein (cornea) and lissamine green (conjunctiva)
- Grade using the Oxford Schema (0–5)
Key patterns:
- Inferior staining → aqueous-deficient dry eye
- Superior involvement → severe evaporative disease
Schirmer’s Test / Tear Meniscus Height
- Schirmer I (with anesthesia): <5 mm = severe deficiency
- Tear meniscus: <0.1 mm suggests low tear volume
Clinical wisdom: TBUT + staining often gives enough direction without full testing.
Step 3: Differentiate Subtype
Once results are gathered, use a simple decision structure:
- TBUT <5 sec + normal Schirmer → Evaporative dry eye (MGD)
- Normal/mild TBUT + low Schirmer → Aqueous-deficient dry eye
- Both abnormal → Mixed type (most common)
Simple Rule
- Poor blinking → evaporative
- Low tear production → aqueous-deficient
- Both → mixed disease
Step 4: Use Advanced Technology Only When Needed
Reserve tools like meibography, osmolarity testing, and biomarkers for:
- Severe unexplained symptoms
- Pre-treatment planning for procedures
- Treatment-resistant cases
Rule: Only test if results will change management.
Step 5: Match Findings to Treatment
Do not treat numbers—treat the patient.
- Low TBUT + gritty feeling → lipid-based artificial tears
- Low Schirmer + redness → cyclosporine/lifitegrast ± punctal plugs
- High staining + contact lens intolerance → switch lens type or consider scleral lenses
Two-Week Review Rule
Reassess in 14 days:
- Improvement → maintain plan
- No improvement → escalate evaluation
Real-World 5-Minute Workflow
- Ask 2 symptom questions
- Perform TBUT
- Check staining
- Estimate tear volume
- Assign subtype + treatment plan
That’s it—five minutes to diagnosis.
Common Pitfalls
- Ignoring lid margin signs (MGD indicators)
- Over-relying on symptoms alone
- Not observing blink patterns in screen users
Final Takeaway
Dry eye diagnosis does not require complex workflows. It requires consistency and structure. With a simple framework—symptom triage, three quick tests, and subtype classification—clinicians can diagnose and treat efficiently within routine consultations.
A simplified system leads to earlier detection, better treatment choices, and improved patient trust.