Senior Eye Doctor Reveals 6 Hidden Causes of Frequent Eye Irritation Beyond Screen Time
If you’ve been rubbing your eyes more than usual, it’s easy to assume your laptop or phone is to blame. But according to a senior eye doctor, that explanation often misses the bigger picture.
Dr. Anushree Sharma, a leading ophthalmologist with over two decades of clinical experience, explains that while screen time contributes to eye strain, it is rarely the sole cause of chronic irritation.
Instead, she identifies six lesser-known factors that frequently drive persistent eye discomfort—many of which go unnoticed in routine self-diagnosis.
The Hidden Culprits Behind Eye Irritation
In clinical practice, many patients arrive having already tried blue-light filters, screen breaks, and lubricating drops—often without meaningful relief.
Dr. Sharma notes that this is because the root cause is frequently environmental, physiological, or even medication-related rather than purely digital strain.
Below are the six most common but overlooked contributors.
1. Dry Indoor Air and HVAC Systems
Modern heating and cooling systems significantly reduce indoor humidity, which accelerates tear evaporation.
Even without obvious dryness in the skin or throat, the eye’s tear film can destabilize quickly.
Common signs include:
- Gritty or sandy sensation in air-conditioned rooms
- Blurred vision that improves after blinking
- Worsening symptoms during winter or prolonged indoor exposure
Practical measures include using humidifiers, preservative-free artificial tears, and taking regular breaks from dry environments.
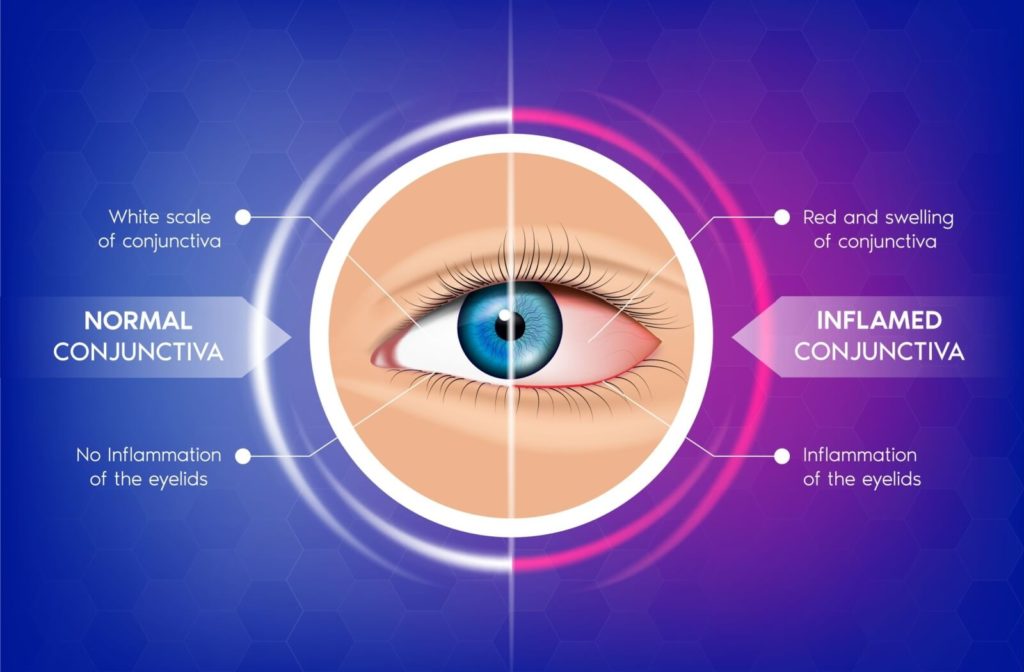
2. Undiagnosed Blepharitis
Blepharitis is chronic inflammation of the eyelid margins and is often mistaken for allergies or fatigue.
Dr. Sharma emphasizes that many patients are unaware they have it.
Typical symptoms include:
- Crust or debris on eyelashes upon waking
- Red or swollen eyelid edges
- Burning or foreign-body sensation
Management usually involves warm compresses, lid hygiene routines, and in some cases, prescription medication.
3. Meibomian Gland Dysfunction (MGD)
MGD affects the oil-producing glands that stabilize the tear film. Without adequate oil, tears evaporate too quickly, leading to chronic irritation.
Dr. Sharma highlights that MGD is increasingly common in younger adults due to reduced blinking during screen use and dietary influences.
Key characteristics:
- Gradual onset of dryness
- Incomplete relief from standard eye drops
- Association with conditions like rosacea or hormonal changes
Treatment may include in-office therapies, omega-3 supplementation, and prescription anti-inflammatory drops.
4. Hidden Airborne Allergens
Low-grade allergic reactions are often overlooked causes of chronic eye irritation.
Common triggers include dust mites, pet dander, mold spores, and accumulated indoor allergens.
High-risk areas:
- Bedding and pillows
- Carpets and upholstered furniture
- Poorly maintained air vents
Reducing exposure through cleaning routines, air filtration, and hypoallergenic bedding can significantly improve symptoms.
5. Nutritional Deficiencies
Eye surface health depends heavily on key nutrients, particularly vitamin A and omega-3 fatty acids.
Deficiencies may contribute to tear instability and inflammation.
Possible signs include:
- Night vision difficulties (vitamin A deficiency)
- Persistent dryness despite eye drops
- Recurrent eyelid inflammation or styes
Dietary sources include leafy greens, carrots, fatty fish, nuts, and seeds, along with supplements when clinically indicated.
6. Medication Side Effects
Several common medications can reduce tear production or alter tear composition.
Dr. Sharma notes that patients often do not associate long-term medication use with eye irritation.
Examples include:
- Antihistamines
- Diuretics
- Antidepressants (SSRIs)
- Acne treatments such as isotretinoin
- Some blood pressure medications
Any suspected medication-related dryness should be reviewed with a physician before making changes.
When to See an Eye Doctor
Occasional irritation after long screen use is common, but persistent symptoms should not be ignored.
Seek professional evaluation if:
- Symptoms last longer than two weeks
- There is pain, light sensitivity, or vision change
- You have autoimmune conditions such as Sjögren’s syndrome
- Symptoms began after starting a new medication
The Bottom Line: Look Beyond the Screen
While digital devices contribute to eye strain, chronic irritation often has deeper underlying causes.
As Dr. Sharma emphasizes, persistent symptoms are rarely due to a single factor. Instead, they usually reflect a combination of environmental stressors, gland dysfunction, nutrition, or medication effects.
Identifying the true cause allows for more targeted treatment—and significantly better long-term relief.