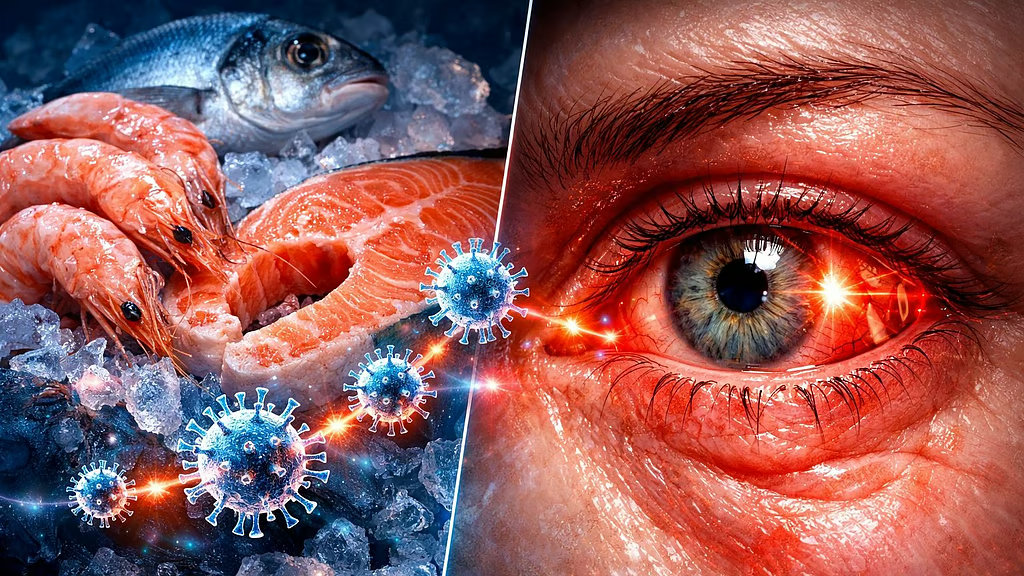
Marine Animal Virus Triggers Rare Eye Disease Outbreak in Humans
In a startling development that blurs the lines between marine biology and human medicine, health experts in India are raising the alarm over a rare but serious eye infection linked to a virus typically found in marine animals. The outbreak, primarily reported in coastal regions, has medical professionals urging for heightened awareness and preventive measures. This unusual crossover event serves as a stark reminder of the intricate and often unpredictable connections within our global ecosystem.
The Unlikely Culprit: A Virus from the Sea
The infection causing concern is known as acute hemorrhagic conjunctivitis (AHC). While conjunctivitis (or “pink eye”) is common and often caused by adenoviruses, this particular severe form is being attributed to the Enterovirus 70 (EV-70). What makes this outbreak remarkable is the suspected origin of the virus.
Recent epidemiological tracing and genetic analysis suggest that the current strain may have a zoonotic origin, meaning it jumped from animals to humans. In this case, the primary reservoirs are believed to be certain marine animals, though the exact species is still under investigation. This isn’t the first time EV-70 has caused problems—it was behind major pandemics of AHC in the 20th century—but its re-emergence with a potential marine link is a new and worrying twist.
Symptoms: More Than Just Pink Eye
This isn’t your typical, mild case of conjunctivitis. Acute hemorrhagic conjunctivitis lives up to its name, presenting with severe and alarming symptoms that require immediate medical attention.
Key symptoms include:
- Sudden Onset of Eye Pain and Redness: The infection begins abruptly, often within 24 hours of exposure.
- Profuse Watering and Swelling: The eyes may become excessively watery and the eyelids significantly swollen.
- The “Hemorrhagic” Sign: The most distinctive feature is spontaneous bleeding under the conjunctiva (the clear membrane covering the white part of the eye), leading to bright red patches.
- Extreme Sensitivity to Light (Photophobia): Patients often find it painful to be in well-lit areas.
- Foreign Body Sensation: A persistent feeling of grit or sand in the eyes is common.
In a small percentage of cases, particularly during past outbreaks, the virus has been associated with neurological complications like polio-like paralysis, making rapid diagnosis and management critical.
How is the Virus Spreading?
The transmission is intensely person-to-person. The virus is highly contagious and spreads through:
- Direct contact with infected eye secretions (e.g., tears, discharge).
- Touching surfaces or objects contaminated with the virus (fomites) and then touching the eyes.
- Close personal contact, such as within households, schools, and healthcare settings.
The marine animal connection is likely at the root of the virus’s introduction into human populations, possibly through environmental contamination of coastal waters or direct handling of infected marine life. Once the jump to humans occurs, it then spreads rapidly through communities via the routes mentioned above.
High-Risk Groups and Geographic Hotspots
The outbreak has shown a distinct pattern. Areas with high population density and close living quarters are most vulnerable. Initial reports have highlighted cases in:
- Coastal Communities: Fishermen, seafood market workers, and those living near contaminated waterways are at the frontline of initial exposure.
- Schools and Hostels: Children and young adults, who may have less stringent hygiene practices, are particularly susceptible to rapid spread.
- Healthcare Workers: Those treating infected patients without proper protective measures are at significant risk.
- Families of Infected Individuals: The virus can sweep through households quickly due to close contact.
Diagnosis, Treatment, and the Challenge of No Vaccine
Diagnosis is primarily clinical, based on the characteristic sudden onset and severe symptoms, especially the hemorrhagic appearance. Laboratory tests, including PCR to detect viral RNA, can confirm the presence of Enterovirus 70.
A significant challenge in managing this outbreak is the lack of a specific antiviral treatment or vaccine for EV-70. Management is purely supportive and focused on:
- Symptomatic Relief: Using cold compresses, artificial tears, and pain relievers (under medical guidance) to manage discomfort.
- Strict Hygiene to Prevent Spread: This is the cornerstone of control.
- Monitoring for Complications: Watching for any signs of neurological issues is crucial.
- Preventing Secondary Bacterial Infection: Doctors may sometimes prescribe antibiotic eye drops if a secondary bacterial infection is suspected.
Prevention: Your Best Defense Against Infection
Given the absence of a vaccine, preventive hygiene measures are the only effective shield against this contagious virus. Health authorities are emphasizing the following:
- Wash Hands Frequently: Use soap and water for at least 20 seconds, especially after touching your face or coming from public spaces.
- Avoid Touching Your Eyes: This is the most important step to break the chain of infection.
- Practice Respiratory and Ocular Hygiene: Use tissues when wiping your eyes and dispose of them immediately. Do not share towels, pillows, or eye makeup.
- Disinfect Surfaces: Regularly clean high-touch surfaces like doorknobs, countertops, and mobile phones.
- Isolate if Infected: Individuals with symptoms should avoid school, work, and public gatherings to prevent community transmission.
- Exercise Caution in Coastal Areas: Those handling marine animals or in areas with suspected water contamination should wear protective gloves and eyewear and wash thoroughly afterward.
The Bigger Picture: A Warning from a Connected World
This outbreak of marine virus-linked eye disease is more than a public health alert; it’s a case study in One Health—the understanding that the health of people is closely connected to the health of animals and our shared environment. Climate change, habitat encroachment, and intensive human activity in coastal ecosystems can disrupt natural balances and facilitate the spillover of pathogens.
The emergence of EV-70 from a marine reservoir is a potent reminder that our health is intertwined with the planet’s. It underscores the need for:
- Strengthened surveillance at the human-animal-environment interface.
- Rapid genomic sequencing to track virus evolution and origin.
- Public education on zoonotic diseases in vulnerable regions.
- Global cooperation in monitoring and responding to such cross-species disease events.
While the current outbreak is being managed through classic public health measures, it sounds a clear alarm bell. In our interconnected world, a virus from the depths of the ocean can find its way to the human eye, reminding us that vigilance, hygiene, and respect for ecological boundaries are our first and best lines of defense.